Linx Vista Glucose Sensor / Linx
Continuous glucose monitoring has fundamentally reshaped the way we understand and manage metabolic health. For decades, glucose control relied on isolated finger-stick measurements, offering only fragmented snapshots of an inherently dynamic process. With the advent of CGM systems, glucose is no longer perceived as a static number, but as a continuous physiological process influenced by food, movement, stress, sleep, medication, and circadian rhythm.
The Linx Vista / Linx glucose sensor belongs to this new generation of technologies designed not only to measure glucose, but to educate, contextualize, and empower users. This master article provides an in-depth, clinically grounded overview of Linx Vista / Linx: how it works, who can benefit from it, how to use it correctly, and—most importantly—how to interpret its data in a meaningful, non-anxious, and actionable way.
Why glucose should be understood as a continuous process
Glucose levels fluctuate constantly. They rise and fall in response to meals, physical activity, stress, hormonal changes, sleep quality, illness, and medication. A single measurement—even if “normal”—cannot capture these variations. Two people may record identical fasting glucose values while experiencing entirely different glycemic profiles throughout the day.
Continuous glucose monitoring shifts the focus from isolated values to patterns, trends, and variability. This shift is crucial because long-term metabolic outcomes are driven not only by average glucose, but also by how much and how often glucose fluctuates.
What is the Linx Vista / Linx glucose sensor
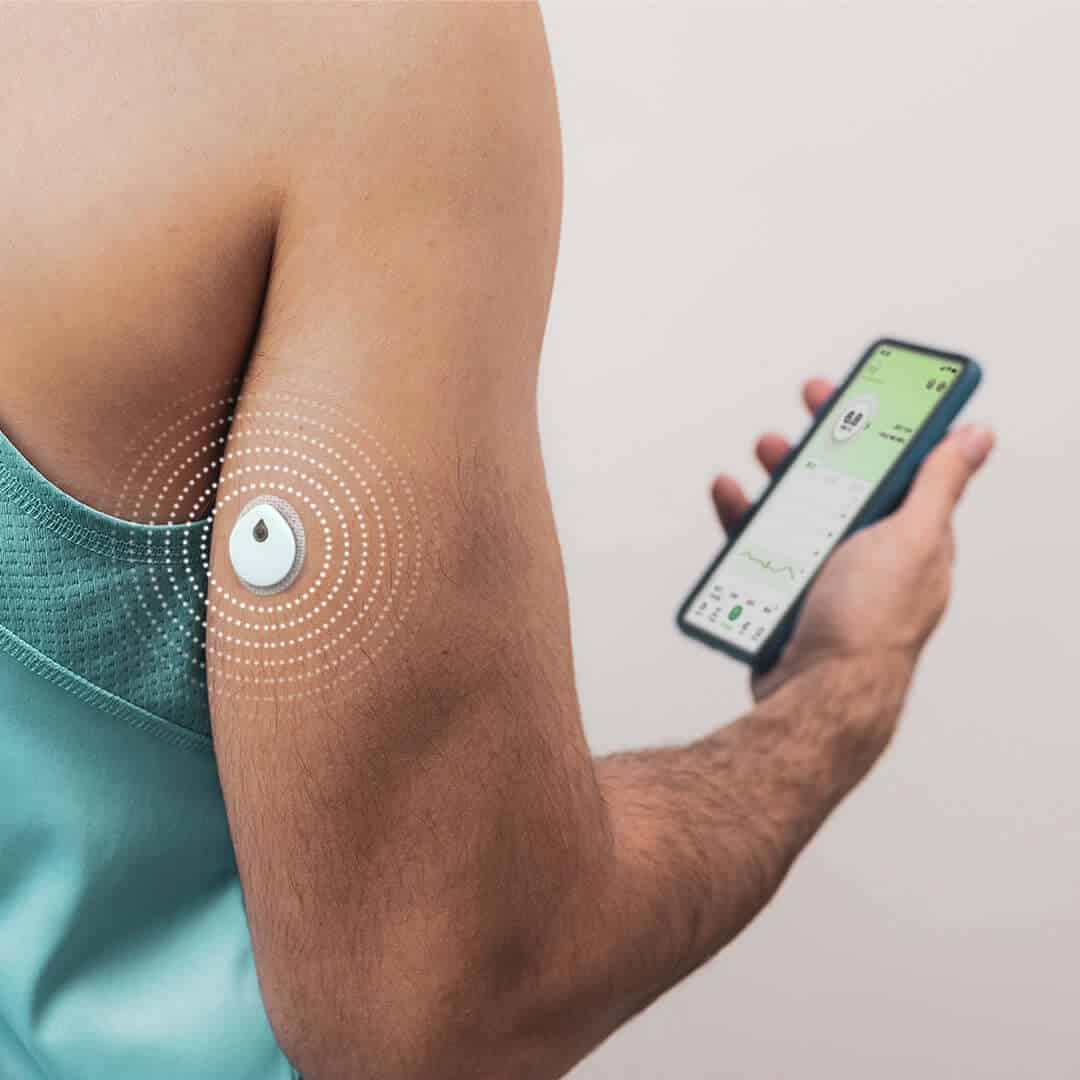
Linx Vista / Linx is a continuous glucose monitoring system that measures glucose concentration in the interstitial fluid, the extracellular compartment into which glucose diffuses from the bloodstream before being taken up by tissues. This method of measurement allows for a dynamic and continuous assessment of glycemic behavior, going beyond the limitations of point-in-time capillary blood glucose measurements. The sensor itself is a small, discreet device designed to be worn comfortably on the skin, most commonly on the upper arm in an area with adequate subcutaneous tissue. Once correctly applied, the sensor remains attached for several consecutive days without requiring daily intervention from the user.
During the wear period, Linx Vista / Linx performs repeated measurements of interstitial glucose at regular intervals using a flexible subcutaneous filament and an electrochemical detection system. The collected data are processed by the sensor’s internal algorithms and transmitted automatically to a compatible mobile application, where they are displayed in an intuitive and accessible format. This continuous transmission enables real-time access to glucose information without the need for active user interaction for each reading.
The true clinical value of the Linx Vista / Linx system lies not merely in the provision of repeated numerical values, but in its ability to construct a continuous glucose curve. This curve illustrates not only absolute glucose levels but also their dynamics, specifically the direction and speed at which glucose is rising or falling at any given moment. As a result, both users and clinicians can gain deeper insight into how the body responds to meals, physical activity, stress, sleep, and therapeutic interventions.
By analyzing the glucose curve, Linx Vista / Linx allows for the identification of clinically relevant patterns, including:
- postprandial glucose excursions and their amplitude,
- nocturnal trends and asymptomatic hypoglycemia,
- recurrent periods of glycemic instability,
- the relationship between therapeutic actions and the resulting glycemic response.
These insights cannot be captured through isolated measurements alone and effectively transform the sensor from a simple measurement device into an advanced metabolic analysis tool. In this context, Linx Vista / Linx supports a more nuanced understanding of glycemic control, enabling better-informed decisions and more refined interventions focused on metabolic stability and predictability rather than on the correction of isolated glucose values.
Foreigner In Romania and in need of a prescription for your chronic treatment?
Contact Dr. Petrache’s Virtual Clinic for any medical issue you encounter while in Romania. Send an email to: [email protected]
What CGM sensors actually measure
Like all continuous glucose monitoring systems, Linx Vista / Linx measures glucose levels in the interstitial fluid, not directly in capillary or venous blood. Interstitial fluid is the extracellular compartment that surrounds the body’s cells and into which glucose diffuses from the bloodstream before being taken up by tissues. Because this transfer is not instantaneous, interstitial glucose reflects blood glucose with a physiological time lag, typically of several minutes.
Under stable metabolic conditions, this delay is minimal and clinically insignificant. However, the lag becomes more apparent during periods of rapid glycemic change, when blood glucose levels are rising or falling quickly. The most common situations in which this physiological delay is noticeable include:
- the postprandial period, especially after meals rich in rapidly absorbable carbohydrates;
- periods of intense or unplanned physical activity, when glucose uptake by muscles increases abruptly;
- episodes of rapidly developing hypoglycemia or hyperglycemia, particularly following insulin corrections or sudden hormonal counter-regulation.
In these contexts, interstitial glucose values may appear temporarily lower or higher than capillary measurements, not because the sensor is inaccurate, but because it is reflecting glucose dynamics in a different physiological compartment. This phenomenon is inherent to human physiology and applies to all CGM systems, regardless of brand or technological sophistication.
It is therefore essential to emphasize that this time lag does not represent a sensor error or malfunction. Rather, it underscores the need to interpret CGM data as a dynamic process, focusing on trends, direction of change, and rate of glucose movement, rather than on rigid, moment-to-moment comparisons with finger-stick measurements. When understood and interpreted correctly, this dynamic perspective is precisely what makes CGM technology a powerful tool for understanding real-world glucose behavior, beyond the limitations of isolated capillary readings.
Who can benefit from Linx Vista / Linx
Although CGM technology was initially developed for people with type 1 diabetes, its use has expanded considerably. Linx Vista / Linx can be valuable for:
- individuals with type 1 diabetes, for hypoglycemia prevention and fine-tuning insulin therapy;
- individuals with type 2 diabetes, including those not treated with insulin;
- women with gestational diabetes, under medical supervision;
- individuals with prediabetes or insulin resistance;
- people interested in metabolic optimization and preventive health.
One of the most powerful insights offered by CGM is metabolic individuality: identical meals can trigger very different glucose responses in different people.
Proper application of Linx Vista / Linx sensor
Correct application of theLinx Vista / Linx sensor is essential to obtain accurate, stable, and clinically meaningful glucose data. Improper application may result in unreliable readings, premature sensor detachment, or local discomfort, which is why this step should never be treated superficially.
The recommended placement site is generally the back of the upper arm, in the upper third, where there is sufficient subcutaneous tissue. This area offers an optimal balance between comfort, sensor stability, and measurement accuracy. Areas with scars, inflammation, irritation, bruising, large moles, or zones exposed to constant pressure—such as areas you frequently lie on during sleep—should be avoided.
Before application, the skin must be thoroughly cleaned with soap and water or an alcohol wipe and allowed to dry completely. It is important that the skin is fully dry and free of creams, oils, sweat, or deodorant, as these can significantly compromise the adhesive. Applying the sensor to damp or oily skin increases the risk of premature detachment.
The Linx Vista / Linx sensor comes with a dedicated applicator equipped with a spring-loaded mechanism. After removing the protective cap, the applicator should be positioned perpendicular to the skin over the selected area. It is important that the applicator is placed firmly and evenly, without tilting. By pressing the applicator button, the spring mechanism quickly and precisely inserts the sensor filament just beneath the skin while securing the sensor in place. The process is very fast and is usually perceived as minimally uncomfortable or even painless.
Once the applicator is removed, the sensor remains attached to the skin via its adhesive patch. The adhesive edges should be gently but firmly pressed for several seconds to ensure proper fixation across the entire surface. This step is particularly important for maintaining sensor stability during movement, sweating, or physical activity.
During the first hours after application, small fluctuations in glucose readings may occur. This is a normal phenomenon related to the sensor’s adaptation to the interstitial environment. During this period, readings should be interpreted cautiously and correlated with overall clinical status, without drawing conclusions or making major adjustments based on isolated values.
A calm, careful, and correct application is the foundation of a successful experience with the Linx Vista / Linx sensor and significantly contributes to the quality and usefulness of the data collected thereafter.
Sensor activation and stabilization period
After application, the Linx Vista / Linx sensor does not immediately display glucose values. It requires an initial warm-up period, which lasts approximately one hour. During this time, the sensor stabilizes and adapts to the interstitial environment—a completely normal process for all continuous glucose monitoring systems.
To start the sensor, the user must install the dedicated Linx Vista / Linx mobile application and create a personal account using an email address. Account creation is necessary for storing and synchronizing glucose data, as well as for accessing glucose history over time. Once logged in, the application provides step-by-step guidance for connecting the sensor.
The smartphone must have Bluetooth enabled, as the Linx Vista / Linx sensor transmits data wirelessly to the app. Once the application detects the nearby sensor, it is automatically paired with the user’s account. During this step, it is important to keep the phone relatively close to the sensor to ensure a stable connection.
After pairing is complete, the warm-up period begins. During this time, the app will display a message indicating that the sensor is initializing and that glucose data are not yet available. No additional action is required from the user during this phase.
Even after the first glucose values appear, it is recommended that the initial hours of readings be interpreted with caution. Mild variability or discrepancies compared with expected values may occur and are part of the normal stabilization process. In the absence of clinical symptoms suggestive of hypoglycemia or hyperglycemia, major therapeutic decisions or corrections should not be based on isolated early readings.
Once the stabilization period is complete, glucose curves become progressively more consistent and predictable. At this stage, the data begin to reflect real glycemic trends more accurately, making the sensor truly useful for daily and medium-term analysis. Understanding this start-up and adaptation process is essential to prevent unnecessary anxiety and misinterpretation during the first days of use.
What the Linx Vista / Linx app provides
The mobile application associated with the sensor represents the central component of the continuous glucose monitoring system. While the sensor itself is responsible for measuring glucose levels, the application is the element that transforms raw data into clinically meaningful information by processing, organizing, visualizing, and contextualizing glucose readings over time.
Through the application, the user has access to:
- real-time glucose values, automatically updated without the need for manual scanning;
- trend arrows that indicate not only the direction but also the speed of glucose changes, which is essential for proper interpretation of the numerical value;
- detailed glucose graphs over short time intervals, such as several hours, useful for assessing postprandial responses or the effects of physical activity;
- longer-term graphs spanning several days, allowing identification of recurring patterns and overall glycemic variability;
- a complete glucose history stored for retrospective analysis;
- the ability to annotate and correlate glucose values with meals, physical activity, medication administration, stress, or other relevant events.
This structured data presentation enables a much more nuanced approach than the simple observation of isolated glucose readings. The application allows users to observe how glucose levels respond to different lifestyle factors, including:
- the composition and timing of meals;
- planned versus unplanned physical activity;
- diurnal versus nocturnal glycemic behavior;
- psychological stress, sleep quality, and routine changes;
- therapeutic interventions and their real-world metabolic impact.
Importantly, the application is not designed to provide automatic therapeutic decisions. Its role is to support understanding rather than dictate action. By presenting glucose data in a dynamic and contextualized manner, the application helps users and clinicians recognize meaningful patterns, distinguish physiological variability from clinically relevant instability, and understand the relationship between daily behaviors and individual glycemic responses.
In this way, the mobile application transforms the CGM system from a simple glucose display into a powerful tool for metabolic education and personalized analysis, supporting more informed, confident, and clinically grounded decision-making.
Why trend arrows matter more than the number itself
A single glucose value can be misleading without context. Trend arrows indicate whether glucose is rising, falling, or stable—and how fast. A glucose value within target range but rising rapidly may require a different response than the same value remaining stable.
Linx Vista / Linx supports proactive decision-making by helping users anticipate changes rather than react after they occur.
Alerts, notifications, and safety
The sensor allows the user to set alerts for glucose values that are too high or too low, as well as for rapid changes in glucose levels indicated by accelerated trends. This alert system plays a critical role in safety, as it can notify the user in situations where active monitoring is limited or symptoms may not be perceived.
Alerts are particularly valuable in specific clinical and real-life contexts, such as:
- during the night, when hypoglycemia may occur without awakening or clear symptoms;
- in individuals with impaired awareness of hypoglycemia;
- during periods of illness, stress, or recent changes in therapy;
- during activities that limit frequent glucose checks, such as driving or physical exertion.
In addition to absolute threshold alerts, alarms based on rapid glucose changes are especially useful from a preventive perspective. They can warn the user of an impending hypo- or hyperglycemic event before glucose levels reach a dangerous range, allowing for earlier and more measured intervention.
Alert configuration should always be individualized, taking into account factors such as the type of diabetes, treatment regimen, history of hypoglycemia, daily routine, and personal tolerance to notifications. Setting thresholds that are too strict or too close to usual glucose values may result in excessive alerts, a phenomenon known as alarm fatigue. Over time, frequent alarms can become intrusive, leading users to ignore notifications or disable them altogether, thereby reducing the protective value of the system.
By contrast, well-calibrated alerts—adjusted gradually based on accumulated data and real-world experience—enhance safety, reduce anxiety, and increase confidence in CGM use. The goal is not to flag every minor deviation, but to identify clinically meaningful situations that truly require attention or action.
When properly understood and configured as tools for warning and prevention rather than rigid control, CGM alerts become a discreet and effective ally in maintaining glycemic balance and supporting long-term, sustainable use of continuous glucose monitoring technology.
Advanced data interpretation: beyond single readings
One of the most common mistakes in the use of continuous glucose monitoring systems is reacting impulsively to every visible fluctuation in glucose values. Glucose is a dynamic physiological variable, influenced continuously by food intake, physical activity, stress hormones, sleep, and treatment effects. As such, short-term variability is not only expected but normal. The clinical objective of CGM use is therefore not the pursuit of perfectly flat glucose lines, but the achievement of overall metabolic stability and the recognition of meaningful patterns.
Focusing excessively on individual readings or minor, short-lived deviations often leads to unnecessary corrective actions and may paradoxically increase glycemic instability. CGM data are most valuable when interpreted in context, with attention to trends, direction of change, and recurrence over time, rather than as isolated numerical events.
Meaningful analysis of CGM data requires reviewing glucose profiles over extended periods, ideally spanning 7 to 14 consecutive days. This timeframe allows for the identification of consistent and reproducible patterns, such as recurrent postprandial excursions, nocturnal hypoglycemia, morning hyperglycemia, or periods of increased variability related to lifestyle factors. In contrast, isolated events—such as a single high or low reading—often reflect transient circumstances and rarely justify major therapeutic changes on their own.
By shifting the focus from short-term fluctuations to medium-term patterns, CGM users and clinicians can better distinguish physiological variability from clinically relevant instability. This approach supports more measured, strategic adjustments and transforms CGM from a source of constant alerts and anxiety into a tool for insight, learning, and sustainable metabolic control.
Passing through Romania and need a prescription for your chronic treatment?
Contact Dr. Petrache’s Virtual Clinic for any medical issue you encounter while in Romania. Send an email to: [email protected]
Linx Vista / Linx limitations
Like any medical device, Linx Vista / Linx has inherent limitations that must be understood in order to interpret its data correctly. The system measures glucose in the interstitial fluid, and its readings can be influenced by a range of physiological, mechanical, and environmental factors. These influences do not represent device malfunction, but rather the interaction between CGM technology and normal biological variability.
Among the most common factors that may temporarily affect sensor readings are:
- dehydration, which reduces interstitial fluid volume and may alter the apparent glucose concentration;
- extreme temperatures, either high or low, which can affect local skin physiology as well as sensor performance and adhesion;
- direct pressure on the sensor, known as compression artifacts, most commonly occurring during sleep or when the sensor is pressed by tight clothing or sustained body positioning;
- certain medications or substances, which may influence glucose metabolism or interfere with the sensor’s electrochemical signal, leading to transient discrepancies.
In such situations, the displayed values may appear unusual or fluctuate unexpectedly without necessarily reflecting true blood glucose levels. For this reason, CGM data should always be interpreted in clinical context and not in isolation.
There are circumstances in which confirmation with a traditional fingerstick glucose meter remains essential, even when using a high-performance CGM system. This is particularly important when:
- symptoms suggestive of hypoglycemia, such as tremor, sweating, confusion, or palpitations, are present but not clearly reflected by the sensor;
- symptoms of significant hyperglycemia occur without corresponding CGM readings;
- extremely low or extremely high glucose values are displayed;
- immediate treatment decisions are required and an additional layer of safety is needed.
Understanding these limitations and using CGM and capillary glucose measurements in a complementary manner allows for a balanced and safe approach to glucose monitoring. When Linx Vista / Linx is used primarily to identify trends and patterns, and fingerstick measurements are reserved for confirmation in specific situations, the two tools work together to support more reliable and clinically sound glycemic management.
Time in Range (TIR): a key modern metric
Time in Range (TIR) represents the percentage of time during which glucose values remain within a predefined target range, most commonly 70–180 mg/dl, with possible adjustments based on age, type of diabetes, treatment modality, risk of hypoglycemia, and individual clinical context. TIR has become one of the most important parameters in modern diabetology because it provides a far more accurate reflection of real-world glycemic stability, rather than relying solely on a retrospective mathematical average.
The clinical relevance of TIR lies in its ability to integrate multiple dimensions of glycemic control simultaneously, including:
- the duration and frequency of hypoglycemic episodes,
- cumulative exposure to hyperglycemia,
- day-to-day glucose variability,
- the functional impact of glucose fluctuations on daily life.
As a result, two individuals may display similar average glucose levels or comparable HbA1c values, yet have fundamentally different metabolic profiles. One may experience wide glucose excursions with frequent highs and lows, while the other maintains relatively stable glucose levels within the target range for most of the day. From a clinical perspective, these two scenarios are not equivalent, and reliance on averages alone may obscure meaningful metabolic risk.
Continuous glucose monitoring makes this distinction visible, and Linx Vista / Linx provides a clear, intuitive representation of the time spent within the optimal range, below range, and above range. Through TIR analysis, both users and clinicians can identify:
- periods of consistently good glycemic control,
- recurrent times of day associated with glucose excursions,
- the relationship between meals, physical activity, stress, and glucose dynamics,
- the real-world effectiveness of therapeutic or nutritional interventions.
An increase in TIR is associated, according to clinical data, with a reduced risk of long-term microvascular complications and with lower exposure to hypoglycemia, including nocturnal episodes. Beyond long-term outcomes, a higher TIR translates into tangible daily benefits such as fewer symptoms, fewer disruptive alarms, greater metabolic predictability, and an overall improvement in quality of life.
From a practical standpoint, TIR represents a more intuitive and actionable goal than metrics based solely on average glucose values. An increase in Time in Range of approximately 5–10% over several weeks is considered clinically meaningful and often reflects a genuine improvement in glycemic stability, even in the absence of dramatic changes in mean glucose levels.
In this context, Time in Range becomes a central tool for assessing and optimizing glycemic control, and its integration into data analysis with Linx Vista / Linx supports a more nuanced, personalized, and clinically relevant understanding of everyday metabolic behavior.
Glycemic variability: the hidden risk factor
Glycemic variability describes the amplitude of glucose fluctuations. Large swings—even with acceptable averages—are Even when average glucose values are considered acceptable, increased glycemic variability can have a significant negative metabolic impact. Repeated fluctuations between higher and lower glucose levels are associated with oxidative stress, chronic low-grade inflammation, and endothelial dysfunction—mechanisms known to contribute to the development and progression of metabolic and vascular complications. This explains why some individuals may appear well controlled when assessed using average glucose values or HbA1c, yet still carry an increased metabolic risk. Without a continuous glucose monitoring system, this variability often remains undetected, as point-in-time measurements fail to capture the true day-to-day and nocturnal dynamics of glucose regulation.
Linx Vista enables precise identification of periods characterized by increased glycemic instability, making visible patterns that might otherwise go unnoticed, even when absolute glucose values do not initially appear alarming. The most common time frames associated with instability include:
- mornings, in the context of the dawn phenomenon, when counter-regulatory hormone secretion leads to progressive glucose elevation;
- postprandial periods, particularly after meals rich in rapidly absorbable carbohydrates;
- intervals of psychological stress or sleep deprivation, which influence glucose regulation through activation of the cortisol–catecholamine axis;
- episodes of intense or unplanned physical activity, which may result in rapid glucose declines followed by compensatory increases.
Continuous monitoring allows not only the recognition of these vulnerable periods, but also a detailed characterization of glycemic variability through assessment of:
- the amplitude of glucose excursions;
- the speed of glucose rises and declines;
- the cumulative time spent outside the target range;
- the recurrence of these instability patterns across multiple days.
From a clinical perspective, reducing glycemic variability represents a realistic, sustainable, and often more meaningful goal than attempting to “force” perfect glucose values at every moment. Stabilizing the glucose curve—even in the absence of dramatic changes in average glucose—has been associated with lower metabolic risk, fewer hypoglycemic episodes, and improved treatment tolerability.
In everyday practice, a strategy focused on variability reduction supports more refined and individualized interventions, targeting meal composition, timing and type of physical activity, and stress management rather than aggressive corrections of isolated readings. In this way, Linx Vista / Linx becomes an essential tool for understanding real-world metabolic dynamics and for achieving a more stable, predictable, and durable form of glycemic control over the long term.
Nocturnal glucose patterns
One of the most common mistakes in the use of continuous glucose monitoring is reacting impulsively to every displayed value. CGM is not designed to function as a “continuous alarm system” triggering action with each minor fluctuation, but rather as a metabolic analysis tool intended to reveal patterns, trends, and recurring behaviors. Glucose is inherently dynamic, and moderate short-term fluctuations are physiological and expected.
Reacting to every individual reading often leads to unnecessary interventions and may actually increase glycemic instability. CGM data lose much of their value when interpreted in isolation, without considering the direction of change, the rate of glucose movement, and the broader context in which the values occur.
Beyond this tendency to overreact, several other common errors can negatively impact the CGM experience:
- obsessive comparison with fingerstick glucose measurements, without accounting for the fact that the two methods assess different physiological compartments (interstitial versus capillary) and are subject to a normal physiological time lag, particularly during rapid glucose changes;
- overinterpretation of data during the first hours of sensor wear, when the sensor is still stabilizing and readings may be more variable or less predictive;
- ignoring metabolic context, such as recent meals, food composition, physical activity, emotional stress, sleep deprivation, or medication timing;
- repeated and excessive corrective actions, based on isolated readings, which can trigger cycles of overcorrection and undercorrection, increasing glycemic variability and hypoglycemia risk.
These errors often arise from a desire for tight control or from limited understanding of how CGM data should be interpreted. In reality, continuous glucose monitoring becomes truly valuable when approached with perspective and patience, focusing on medium-term trends rather than momentary deviations.
Understanding these pitfalls is essential for a positive and effective CGM experience. When used as a tool for learning and analysis rather than constant surveillance, CGM supports calmer decision-making, reduces anxiety, and contributes to more stable and sustainable glycemic control over time.
Linx Vista / Linx in type 1 diabetes
For people with type 1 diabetes, CGM is both a safety and optimization tool. Linx Vista supports:
- early detection and prevention of hypoglycemia,
- basal and bolus insulin fine-tuning,
- assessment of meal composition effects,
- increased confidence during daily activities and exercise.
Trend arrows are particularly valuable for anticipating rapid glucose changes and avoiding over-corrections.
Linx Vista / Linx in type 2 diabetes
In type 2 diabetes, CGM often serves as a powerful educational tool. Many individuals discover for the first time how different foods, meal timing, stress, or inactivity affect their glucose levels.
Linx Vista can reveal:
- significant post-meal spikes after seemingly “healthy” foods,
- differences in glucose response to similar meals,
- the impact of light physical activity,
- stress-related hyperglycemia.
This awareness frequently leads to spontaneous, sustainable behavior change.
CGM in prediabetes and prevention
In prediabetes, Linx Vista / Linx can function as an early warning system. Abnormal glucose patterns become visible before diabetes develops, allowing timely intervention.
Often, small adjustments in meal composition, timing, or activity level result in noticeable improvements within days.
Common interpretation errors
One of the most common mistakes in the use of continuous glucose monitoring is reacting impulsively to every displayed value. CGM is not designed to function as a “continuous alarm system” triggering action with each minor fluctuation, but rather as a metabolic analysis tool intended to reveal patterns, trends, and recurring behaviors. Glucose is inherently dynamic, and moderate short-term fluctuations are physiological and expected.
Reacting to every individual reading often leads to unnecessary interventions and may actually increase glycemic instability. CGM data lose much of their value when interpreted in isolation, without considering the direction of change, the rate of glucose movement, and the broader context in which the values occur.
Beyond this tendency to overreact, several other common errors can negatively impact the CGM experience:
- obsessive comparison with fingerstick glucose measurements, without accounting for the fact that the two methods assess different physiological compartments (interstitial versus capillary) and are subject to a normal physiological time lag, particularly during rapid glucose changes;
- overinterpretation of data during the first hours of sensor wear, when the sensor is still stabilizing and readings may be more variable or less predictive;
- ignoring metabolic context, such as recent meals, food composition, physical activity, emotional stress, sleep deprivation, or medication timing;
- repeated and excessive corrective actions, based on isolated readings, which can trigger cycles of overcorrection and undercorrection, increasing glycemic variability and hypoglycemia risk.
These errors often arise from a desire for tight control or from limited understanding of how CGM data should be interpreted. In reality, continuous glucose monitoring becomes truly valuable when approached with perspective and patience, focusing on medium-term trends rather than momentary deviations.
Understanding these pitfalls is essential for a positive and effective CGM experience. When used as a tool for learning and analysis rather than constant surveillance, CGM supports calmer decision-making, reduces anxiety, and contributes to more stable and sustainable glycemic control over time.
Passing through Romania and need a prescription for your chronic treatment?
Contact Dr. Petrache’s Virtual Clinic for any medical issue you encounter while in Romania. Send an email to: [email protected]
Integrating Linx Vista / Linx data into personalized nutrition
One of the most valuable advantages of continuous glucose monitoring is the ability to build a truly personalized nutrition plan based on an individual’s real metabolic responses rather than on generalized dietary recommendations or population averages. The impact of food on glucose levels is highly individual, and CGM makes it possible to directly observe how the body responds to different foods, combinations, and eating patterns in everyday life.
The data provided by Linx Vista / Linx can clearly demonstrate:
- which foods trigger rapid and pronounced glucose rises, even when those foods are traditionally considered “acceptable”;
- which food combinations are better tolerated, such as pairing carbohydrates with protein, fat, or fiber to blunt postprandial glucose spikes;
- which time windows are optimal for meals, reflecting individual circadian rhythms and variations in glucose sensitivity;
- how portion size influences the glycemic response, with meaningful differences sometimes observed even when the same food is consumed;
- the impact of food order within a meal, such as consuming fiber- or protein-rich foods before carbohydrates.
This approach allows differentiation between foods that produce sharp glucose peaks and those that result in slower, more stable glucose rises, even when caloric or carbohydrate content is similar. CGM also reveals how contextual factors—such as psychological stress, poor sleep, or recent physical activity—can significantly alter glucose tolerance to the same meal on different days.
Based on these insights, nutritional strategies can be refined through:
- adjusting the type and quality of carbohydrates consumed;
- optimizing food combinations;
- modifying meal timing;
- individualizing portion sizes;
- aligning dietary choices with physical activity and treatment regimens.
As a result, nutritional recommendations shift from being generic and restrictive to being personalized, flexible, and sustainable, tailored to each individual’s physiology. Linx Vista / Linx thus transforms nutrition from a source of uncertainty into a powerful tool for metabolic understanding, supporting informed choices that promote glycemic stability and a healthier, more balanced relationship with food over the long term.
Physical activity through the CGM lens
Physical activity is one of the most powerful modulators of glucose levels, exerting a direct and often rapid influence on how the body utilizes glucose. Exercise affects both insulin sensitivity and glucose uptake by skeletal muscle through insulin-independent pathways, which explains why its effects can be observed even without changes in medication. Continuous glucose monitoring with Linx Vista makes these effects visible in a way that cannot be captured by isolated measurements.
CGM data allow clear differentiation of the glycemic impact of various types of physical activity, revealing distinct response patterns depending on intensity, duration, and timing. Common examples include:
- light postprandial walking, which can reduce the height of post-meal glucose peaks and accelerate the return to the target range;
- resistance or strength training, which may initially cause a transient rise in glucose due to counter-regulatory hormone release, followed by improved insulin sensitivity over time;
- sustained aerobic activity, which typically leads to a gradual glucose decline and an increase in time spent within the optimal range;
- prolonged sedentary behavior, associated with slow but persistent glucose elevations and increased metabolic variability.
A key advantage of CGM use is the ability to observe the effects of even small behavioral interventions. Many users discover that short bouts of movement—often as little as 5 to 15 minutes—can have a meaningful impact on the glucose curve, particularly when strategically timed after meals or during periods of rising glucose.
By analyzing these individualized responses, physical activity can be used not merely as a general lifestyle recommendation, but as a personalized metabolic tool. Linx Vista / Linx enables users and clinicians to tailor the type, timing, and duration of exercise based on real glucose responses, transforming movement from an abstract obligation into a precise and effective metabolic intervention.
Psychological aspects of CGM use
An often underestimated aspect of continuous glucose monitoring is its emotional and psychological impact on the user. For some individuals, constant access to glucose data provides reassurance, a sense of safety, and greater perceived control, particularly by reducing fear of unexpected hypoglycemic or hyperglycemic events. For others, however, the same continuous stream of information can become overwhelming and may trigger anxiety, hypervigilance, or excessive self-monitoring.
The difference between these experiences is not determined by the technology itself, but by how the data are understood and interpreted. Continuous access to glucose values, alerts, and graphs—when not accompanied by adequate education—can create a sense of constant evaluation or the perception that every fluctuation represents a failure. This mindset may increase stress, promote impulsive corrective behaviors, and negatively affect the individual’s relationship with their own body and with diabetes management.
Education and clinical guidance are therefore essential in shaping a healthy relationship with CGM data. Understanding that glucose variability is normal, that there is no such thing as a “perfect” glucose curve, and that data should be analyzed over time rather than moment by moment fundamentally changes the user experience. When individuals learn to interpret CGM data as information rather than judgment, emotional pressure is significantly reduced.
In this context, Linx Vista / Linx should be viewed as a tool for learning and metabolic self-awareness, not as a mechanism of evaluation or self-criticism. Its purpose is not to label behaviors as “good” or “bad,” but to provide objective feedback on how the body responds to food, physical activity, stress, sleep, and treatment. This perspective encourages curiosity rather than self-blame and supports a more compassionate, realistic approach to glucose management.
When supported by appropriate education and professional guidance, CGM technology can actually reduce anxiety rather than intensify it. Used correctly, Linx Vista / Linx has the potential to strengthen confidence, promote calmer and more informed decision-making, and support more stable metabolic control—precisely because it offers understanding, not pressure.
Limitations and when confirmation is needed
Despite the many advantages of continuous glucose monitoring, there are specific situations in which finger-stick blood glucose confirmation remains important and clinically appropriate. CGM systems are designed to provide trends, patterns, and contextual insight rather than to fully replace capillary measurements in every scenario. Recognizing when confirmation is needed is a key component of safe and confident CGM use.
Finger-stick verification is particularly important in situations such as:
- the presence of symptoms that are inconsistent with CGM readings, for example when an individual experiences signs suggestive of hypoglycemia or hyperglycemia despite values displayed within or near the target range;
- suspected severe hypoglycemia, especially when rapid clinical decisions are required and an added layer of certainty is necessary;
- unusually extreme CGM values, either very low or very high, which may warrant confirmation before corrective action;
- the first hours after sensor application, during the initial stabilization phase, when readings may be more variable as the sensor adapts to the interstitial environment.
In these contexts, finger-stick measurements serve as a complementary safety tool rather than a contradiction of CGM technology. Importantly, the need for confirmation does not imply sensor failure or unreliability. Instead, it reflects the physiological reality that CGM measures glucose in the interstitial compartment and is subject to normal biological and temporal variability.
Understanding these limitations and using finger-stick testing selectively—rather than compulsively—actually strengthens trust in CGM technology. When users know when and why confirmation is appropriate, they are less likely to doubt the system unnecessarily and more likely to interpret CGM data with confidence and perspective.
In this balanced approach, CGM provides continuous insight into glucose trends and patterns, while finger-stick measurements remain a targeted tool for safety in specific situations. Together, they support informed decision-making, reduce uncertainty, and promote a more secure and effective use of glucose monitoring technology.
Tourist in Romania and in need of a prescription for your chronic treatment?
Contact Dr. Petrache’s Virtual Clinic for any medical issue you encounter while in Romania. Send an email to: [email protected]
Linx Vista / Linx – most common errors
The most common errors in the use of continuous glucose monitoring systems are not related to the technology itself, but to how the data are interpreted and acted upon. One of the most frequent mistakes is reacting to every minor fluctuation. Glucose levels are inherently dynamic, and small short-term variations are physiological and expected. Treating every deviation as a problem requiring intervention leads to a reactive mindset and obscures the broader picture of metabolic control.
A direct consequence of this overreactive approach is the tendency toward repeated overcorrections. Frequent corrective actions based on isolated readings can trigger a vicious cycle of over- and under-correction, increasing glycemic variability and raising the risk of hypoglycemia. Rather than stabilizing glucose levels, such behavior often makes them more erratic and harder to manage.
Another important error is ignoring trends in favor of single point values. CGM data should always be interpreted together with trend arrows and the overall glucose curve. A value that appears acceptable may actually signal risk if accompanied by a rapid upward or downward trend, while a value slightly outside the target range may not require intervention if the trend is stable and the clinical context is appropriate. Focusing solely on numbers without considering direction and velocity significantly limits the clinical usefulness of CGM.
A further common pitfall is misinterpreting artifacts as real glycemic events. Phenomena such as compression artifacts during sleep or transient variability in the first hours after sensor application can produce readings that do not reflect true blood glucose levels. Treating these artifacts as genuine events may lead to unnecessary interventions and confusion.
These errors most often arise in the absence of a clear understanding of how CGM systems work and what their limitations are. For this reason, user education and medical guidance are essential in preventing such situations. Effective CGM use requires learning to:
- analyze data over longer time frames rather than moment by moment;
- prioritize trends and recurring patterns over isolated readings;
- recognize when intervention is unnecessary;
- distinguish normal physiological variability from clinically meaningful instability.
When these principles are well understood, CGM becomes a powerful tool for metabolic analysis and learning rather than a source of confusion or stress. Appropriate medical guidance transforms raw data into actionable insight, supporting calmer decision-making, improved safety, and more stable long-term glycemic control.
Linx Vista / Linx as a long-term metabolic education tool
Over the long term, continuous glucose monitoring contributes to a fundamental shift in the individual’s relationship with glucose values. Rather than being perceived in a binary framework as “good” or “bad,” glucose data gradually become understood as neutral, informative signals that provide insight into how the body responds to everyday influences.
This change in perspective is essential because it reduces the emotional burden attached to individual readings. Glucose values are no longer experienced as judgments or personal evaluations, but as biological information reflecting the complex interaction between nutrition, physical activity, stress, sleep, treatment, and individual physiology. Within this framework, fluctuations are not automatically interpreted as failures, but as opportunities for understanding and adjustment.
As familiarity with personal glucose patterns increases, CGM supports the development of a more balanced and realistic approach to glycemic management. This shift is often associated with:
- reduced anxiety related to isolated glucose values;
- increased confidence in daily decision-making;
- greater acceptance of physiological variability as a normal part of life;
- a focus on trends and progress rather than on perfection.
This reframing has a direct and meaningful impact on long-term adherence. When monitoring is no longer experienced as a source of pressure or self-criticism, individuals are more likely to continue using the sensor consistently, engage thoughtfully with their data, and implement sustainable changes over time. Motivation becomes driven by curiosity, autonomy, and understanding rather than fear or guilt.
Ultimately, this shift in mindset represents one of the most valuable contributions of CGM technology. By transforming glucose values from a judgment-laden metric into an objective feedback tool, CGM creates the conditions for more stable, flexible, and realistic metabolic management. It is precisely this mature relationship with data that supports durable outcomes and an improved quality of life over the long term.
Final conclusion
The Linx Vista / Linx glucose sensor is far more than a measurement device. It is a tool for understanding, education, and prevention. When used correctly and interpreted in context, it can profoundly change how individuals manage diabetes and metabolic health.
Success does not come from obsessing over every number, but from recognizing patterns, reducing variability, increasing time in range, and integrating insights into a personalized, medically guided plan.
Follow us on:
- FaceBook: Diabetes & Nutrition;
- YouTube: Diabetes Facts.
















